
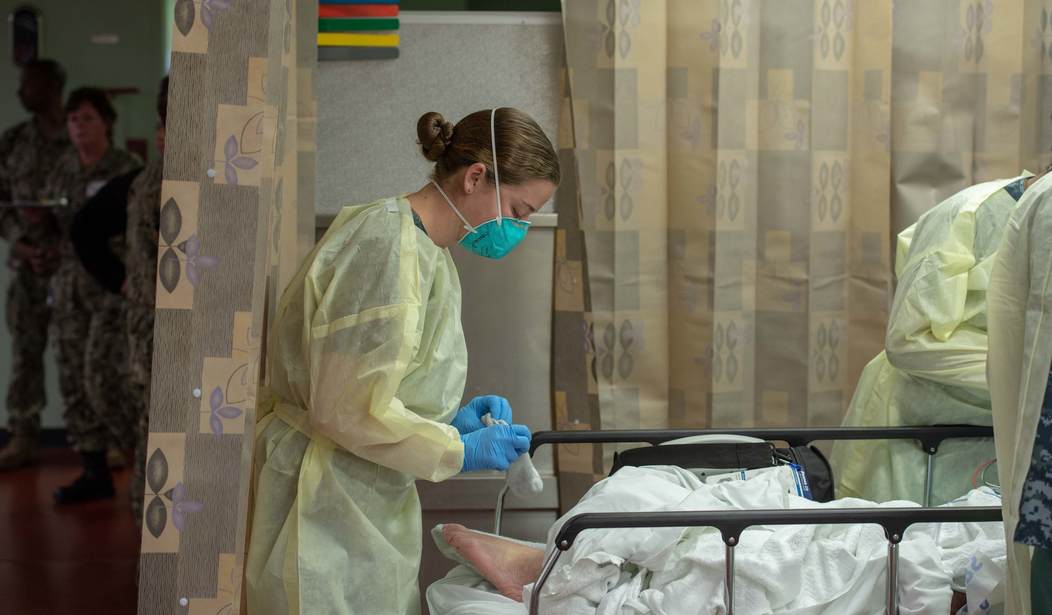
LOS ANGELES (March 29, 2020) Sailors assigned to the hospital ship USNS Mercy (T-AH 19) treat a patient from Los Angeles medical facilities March 29. Mercy deployed in support of the nation’s COVID-19 response efforts, and will serve as a referral hospital for non-COVID-19 patients currently admitted to shore-based hospitals. This allows shore base hospitals to focus their efforts on COVID-19 cases. One of the Department of Defense’s missions is Defense Support of Civil Authorities. DoD is supporting the Federal Emergency Management Agency, the lead federal agency, as well as state, local and public health authorities in helping protect the health and safety of the American people. (U.S. Navy photo by Mass Communication Specialist 2nd Class Erwin Jacob Miciano)
The novel coronavirus (COVID-19) has brought the world to its knees. As this deadly virus spreads throughout the globe, entire countries have shut down to slow its spread. These “shelter at home” orders were issued by governments to avoid flooding hospitals and overwhelming limited medical capacity.
In many states, this capacity has been artificially lowered and the ability to increase capacity inhibited by certificate of need (CON) laws. These laws currently exist in 35 states and the District of Columbia.
In 1964, CON laws were introduced in New York. At the time, they were justified based on faulty reasoning that inverted the economic law of supply and demand. Proponents argued that instead of excess capacity (supply) in a system lowering prices, it would cause increased costs from the maintenance of unused medical facilities. By embracing this flawed reasoning, proponents shepherded the common canard that health care is the one industry immune to the principles of economics. Instead, they called for centrally controlled, government-authorized restriction on medical capacity enshrined in CON laws.
Worse, the boards that oversee and administer CON laws frequently include existing competitors against whom new capacity would contend with. This allows existing hospitals and medical providers to exclude competitors from the market. This functionally shields existing health care service providers and hospitals from higher quality, lower cost competition via the government-sanctioned monopoly of the — not ironically named — CON.
CON laws have also resulted in the development of an unexpected market: the market for acquiring certificates of need. After the enactment of CON laws, health care entities began buying and selling government CON certificates like a commodity. This is due to the fact that not having one is the kiss of death for any new or expanding medical facility. For example, radiology groups desiring new MRI scanners may buy up smaller groups that they have no interest in solely for the purpose of acquiring their CON certificate. This functionally gives a substantial monetary value to a government certificate.
CON laws can also affect the availability of physical facilities as existing facilities are rendered immediately worthless when the owner of the CON transfers the certification to a new facility. This renders legally unusable otherwise perfectly functional facilities solely because they lack the government’s CON blessing.
The expense of acquiring a CON is substantial. It is so substantial that it prices many medical service providers entirely out of the market. Despite significant capital and time investment, obtaining a CON remains uncertain. Approval is subject to the whim of those in government and requires obtaining political favor. Thus, in a very un-American fashion, the creation of new facilities has become so arbitrary, so costly, and so time-consuming that it now becomes the sole purview of the wealthy and politically connected.
Finally, COVID-19 has exposed yet another flaw in this ultimate crony law. CON laws have made consumers vulnerable to a sudden increase in medical demand and thus endanger public health. By artificially restricting the bed capacity of a region, CON laws have made the public susceptible to the legitimate risk of exceeding a community’s ability to respond to pandemics like the coronavirus.
This is why, during this time of intense medical need, states need to learn from the mistakes of the past, free our medical innovators, and reverse these anti-competitive, dangerous, and totally unnecessary certificate of need laws.
Chad Savage, M.D. ([email protected]) is a health care policy advisor for The Heartland Institute and founder of YourChoice Direct Care in Brighton, Michigan












Join the conversation as a VIP Member